Executive Summary
This 9-month case study demonstrates how Sound Blanket™ helped a high-risk skilled nursing community reduce falls, behaviors, and psychotropic medication use — all without increasing staff burden. Drawing on Minimum Data Set Quality Measures (MDS QMs), Quality Assurance and Performance Improvement (QAPI) metrics, and direct staff feedback, the results highlight a scalable, non-pharmacological solution for a dementia population in skilled nursing care settings that not only improved outcomes — Sound Blanket™ led to sustained directional reversals across all areas measured.
Background

Deerfield Episcopal Retirement Community (DERC) is a mission-driven senior care organization in Asheville, NC. Known for serving an older-than-average population with complex care needs, DERC partnered with Composure to implement Sound Blanket™ to target resident sleep quality as a modifiable risk factor and root cause of negative clinical outcomes.
This case study includes a 3-month baseline period followed by a 6-month implementation phase, evaluating MDS QMs and QAPI data from a Pre/Post perspective as well as stand-alone staff survey data as a snapshot in time from the middle of implementation.
At a Glance
Median changes from pre to post
- 1450% improvement in behavior-related measures
- 152% directional improvement in fall-related measures
- 214% improvement in antianxiety/hypnotic use
- 182% improvement in antipsychotic use
- 100% of staff reported no increases in workload
Outcome Details
To reduce the impact of transient, outlier data, all figures below represent the median values compared to DERC’s historical average for each measure.
-
Prevalence of Falls
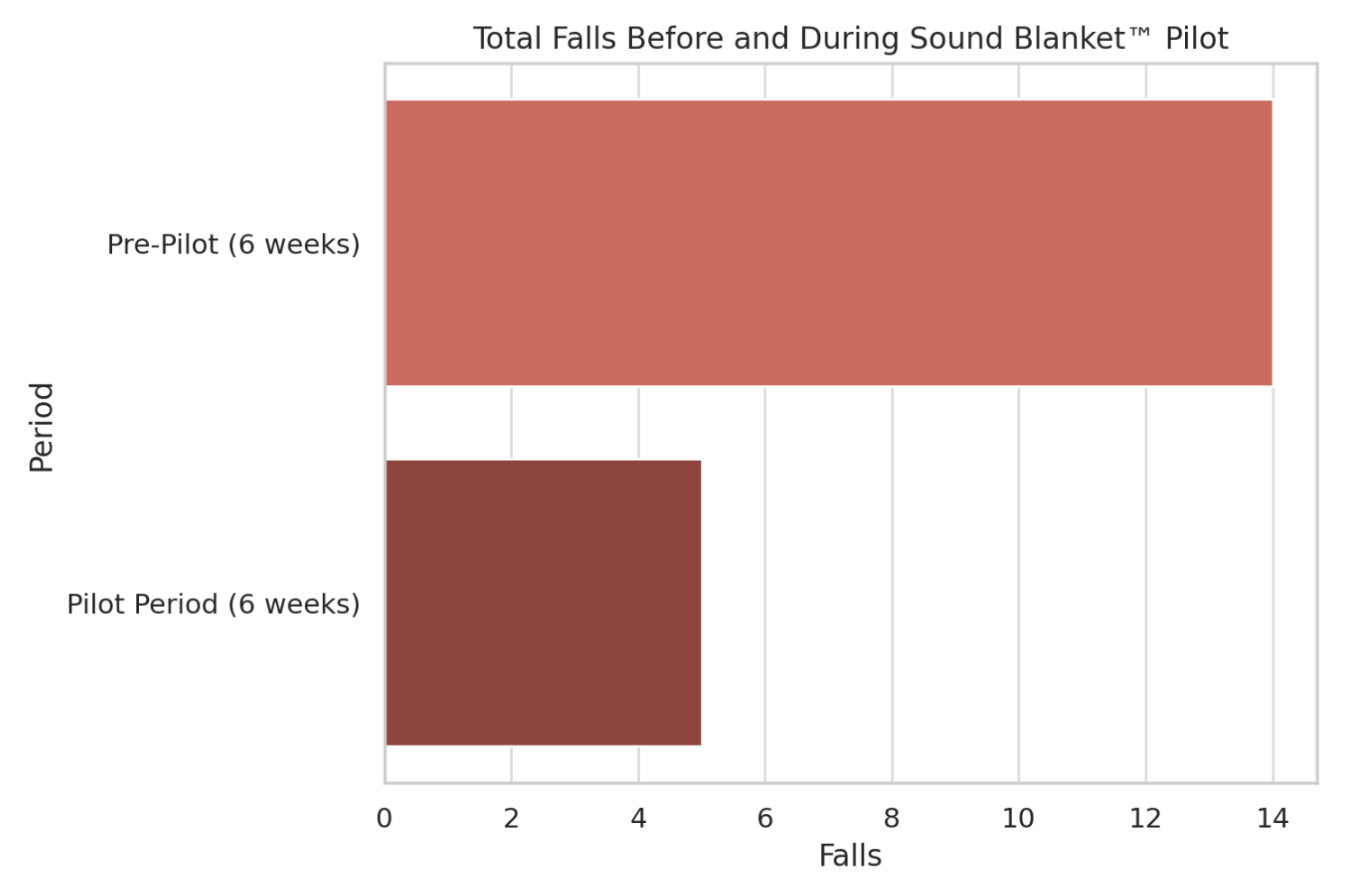
- The prevalence of falls pre-intervention was 4.9% above historical average and improved to 2.6% below during post-intervention. This represents a 152% directional improvement from pre to post.
-
Behavior-Related Quality Measures
- Regarding resident behaviors that impact other residents and/or staff, pre-intervention behaviors were 0.4% above the historical average, and post-intervention behaviors fell to 5.3% below the historical average. Result? A clear and complete reversal in the prevalence and severity of behavioral expressions from pre to post, reflecting consistent and sustained behavior stabilization. Additionally, staff survey data reflected fewer disturbances, better engagement, and more alertness observed during the day.
-
Antipsychotic Use
- The use of antipsychotics shifted from 5.8% above historical average during the pre-intervention period, to 4.8% below during the post-intervention period, resulting in a 150% improvement in trend from pre to post.
- Antianxiety/Hypnotic Use
- Even more dramatic was the change in antianxiety and hypnotics use from 10.6% above to 12.1% below the historical average from pre to post. An astounding 214% improvement is reflected, drastically reducing the need for sleep-related pharmacologic interventions.
Pre/Post vs Historical Average
Pre/Post: Falls, Behaviors, Psychotropics
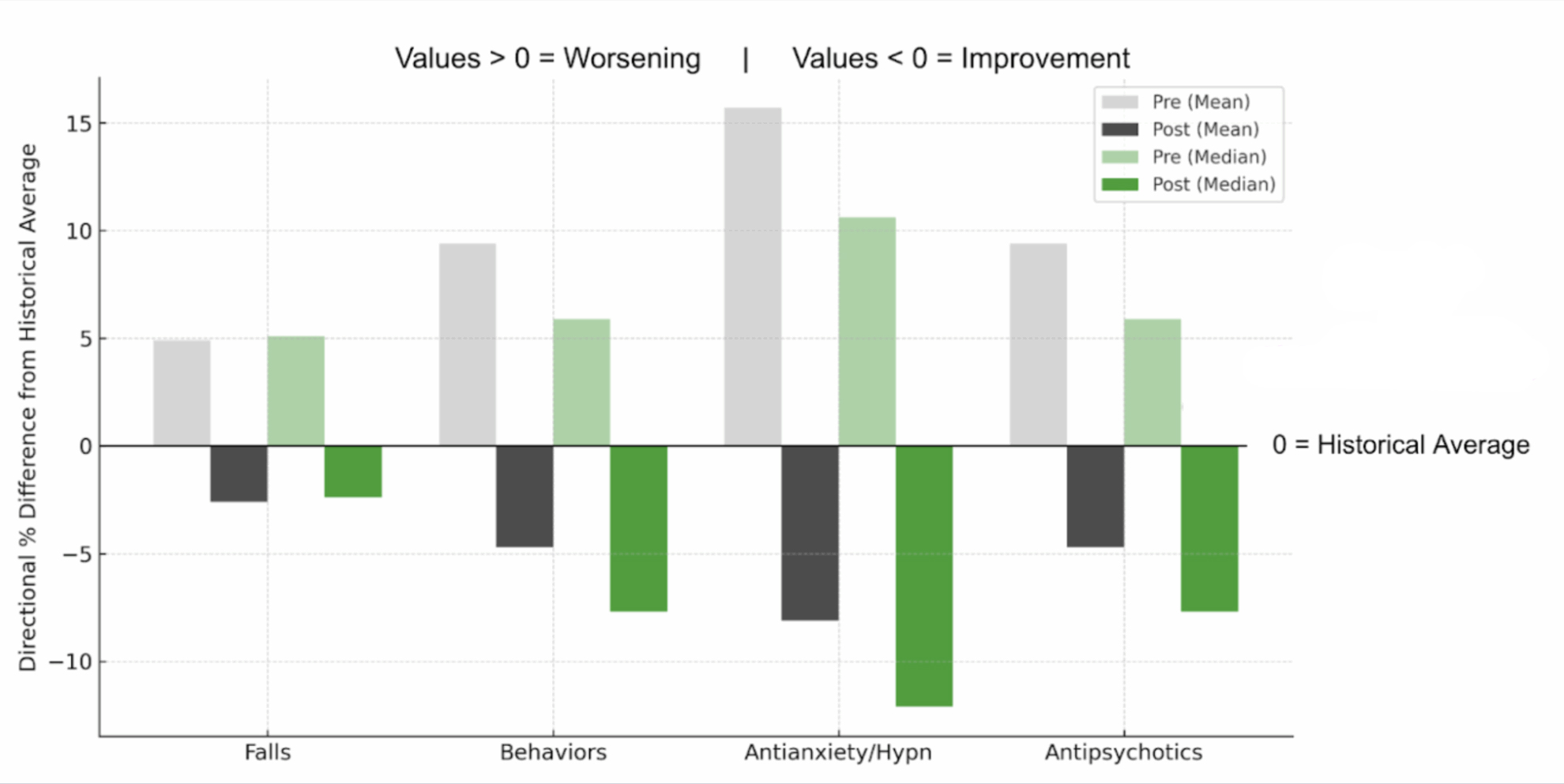
The chart above reflects an average of 44 residents per month. The middle line (“0”) represents Deerfield’s historical average for each measure, while bars above and below show the pre- and post- (for both the mean and median) in relation to that historical average baseline.
Staff Feedback – Sound Blanket™ is High Impact with Zero Burden
Two separate staff surveys were conducted during the first 6 months of Sound Blanket™ implementation reinforcing the intervention’s continued impact and highlight new opportunities for refinement.
- 67% of staff reported residents were sleeping more soundly
- 80% observed less nighttime disruption
- In both survey rounds, 100% of staff reported no increases in workload
“Sound Blanket™ has been a wonderful addition to our efforts to create an environment for our residents that gives them the best opportunity for quality-of-life improvements while dealing with their unique health challenges. We are grateful for the relationship.”
Brian King, Director of Health Services at Deerfield Episcopal Retirement Community
Why This Matters
- Improves survey readiness: Reductions in behaviors, medication use, and falls address high-priority CMS quality domains.
- Strengthens QAPI: Supports a clear, data-backed improvement narrative for internal and external stakeholders.
- Eases operational pressure: Demonstrates measurable improvement without additional staff or pharmacological interventions.
What’s Next

Deerfield and Composure will continue data collection through a full 12-month study period (Part 2). Select residents may also be evaluated using passive bed sensors (such as the Withings Sleep Mat) to gather objective sleep metrics, providing baseline insights to help tailor interventions to individual sleep profiles.
While most residents adapted well to Sound Blanket™, feedback suggests that those who are more alert and verbally expressive may have unique preferences. This highlights the importance of proactively assessing sleep needs and supports the value of integrating objective monitoring tools into the onboarding process.
In response, Deerfield and Composure discussed offering greater resident agency with a simple, resident-friendly controller app to personalize or opt out of the soundscape. While still under consideration, this concept reflects a commitment to honoring person-centeredness and advancing non-pharmacological care strategies.
Ready to explore Sound Blanket™ for your community? Book a 30-minute consultation
Contact us: sales@composure.care